Clients with some types of personality disorders do not exhibity insight for their condition and are unlikely to seek treatment. They often go undiagnosed unless they seek treatment for another psychiatric or medical diagnosis. Some may also be forced to seek treatment at the influence of family members or as required by law if legal infractions have occurred. Personality disorders can be challenging for mental health professionals to treat. Individuals with personality disorders struggle to recognize that their difficulties in life are related to their personalities. They may truly believe their problems are a result of other people or outside factors. It is very common for clients with personality disorders to also have substance abuse, anxiety, depression, or eating disorders.[1]
Psychotherapy is the first line of treatment for personality disorders. Medications may also be prescribed to treat underlying co-occurring conditions such as anxiety or depression.
Psychotherapy
During psychotherapy, an individual can gain insight and knowledge about the personality disorder and what is contributing to their symptoms. They talk about their thoughts, feelings, and behaviors and ideally will develop an understanding of the impact of their thoughts and behaviors on themselves and others. They learn strategies for managing and coping with their symptoms. This treatment can help reduce problematic behaviors that impact an individual’s relationships and functioning.[2]
Common types of psychotherapy used to treat personality disorders are as follows[3]:
- Cognitive behavior therapy
- Dialectical behavior therapy
- Interpersonal therapy
- Psychoanalytic/psychodynamic therapy
- Psychoeducation
Cognitive behavior therapy (CBT) teaches the client to become more aware of the way they think so they can ultimately change the way they behave.
Dialectical behavior therapy (DBT) is a type of cognitive behavioral therapy that was originally created for clients with borderline personality disorder to help them cope with stress, control emotions, and establish healthy relationships. It is considered the gold standard for treating borderline personality disorder and is also used for other types of disorders. The client learns how to be aware of how thoughts, feelings, behaviors link together. They learn how to use their senses to be aware of what is happening around them and how to use strategies (such as mindfulness, distress tolerance, interpersonal effectiveness, and emotion regulation) to react calmly in a crisis, avoid negative impulsive behavior, and improve relationships.[4] See Figure 10.11[5] for an illustration of how thoughts, feelings and behaviors are linked together.
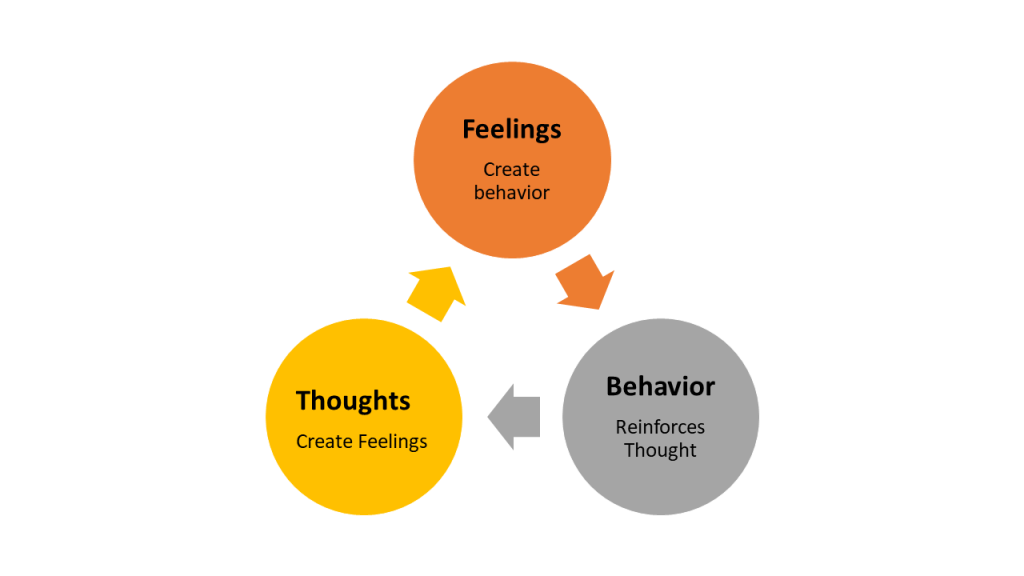
Interpersonal therapy focuses on developing healthy relationships with others. Negative aspects of relationships, such as social isolation and aggression, are identified, and strategies to improve relationships are discussed and planned.
Psychodynamic therapy promotes self-reflection and self-examination of problematic relationship patterns and unresolved conflicts. It can bring awareness of how one’s past has an influence on one’s present behavior.
Psychoeducation teaches the client about their medications, psychotherapies, and support groups available in the community. Wraparound services may be planned with an individualized plan of care that brings multiple services/supports together for the client.
Pharmacotherapy
There are no specific medications approved to treat personality disorders. However, clients who have severe symptoms may be prescribed medications as off-label use that are not necessarily approved by the U.S. Food and Drug Administration (FDA) for personality disorders but are guided by expert opinion and experience. The decision to treat an individual with a personality disorder with medication should be made through shared decision-making with the client based on drug efficacy for their symptoms, potential adverse effects, and their degree of impairment.[6]
Symptom domains that cause impairment and distress across personality disorders and medications commonly used to treat them include the following[7]:
- Cognitive-perceptual symptoms (e.g., hallucinations and paranoid ideation): Treated with low-dose antipsychotics such as aripiprazole, risperidone, and quetiapine.
- Impulsive behaviors (e.g., self-injury, theft, interpersonal conflict): Treated with mood stabilizers (such as lithium and lamotrigine). Omega-3 is used as an adjunct to treat clients who demonstrate recurrent self-harm.
- Affective dysregulation (e.g., depressed mood, mood lability, anxiety, anger): Treated with low-dose antipsychotics and mood stabilizers.
Some guidelines apply to medications prescribed to clients with personality disorders for safety reasons. For example, medications that can be fatal in overdose should be avoided, as well as those that can induce physiological dependence and tolerance. Benzodiazepines can be especially toxic when combined with alcohol or opioids, and they can also cause behavioral disinhibition in patients with personality disorders.[8] Nurses should keep these safety guidelines in mind when teaching clients about their medications.
- Halter, M. (2022). Varcarolis’ foundations of psychiatric-mental health nursing (9th ed.). Saunders. ↵
- American Psychiatric Association. (n.d.). What are personality disorders? https://www.psychiatry.org/patients-families/personality-disorders/what-are-personality-disorders ↵
- American Psychiatric Association. (n.d.). What are personality disorders? https://www.psychiatry.org/patients-families/personality-disorders/what-are-personality-disorders ↵
- Schimelpfening, N. (2021, November 5). What is dialectical behavior therapy (DBT)? Verywell Mind. https://www.verywellmind.com/dialectical-behavior-therapy-1067402 ↵
- "Dialectical Behavior Therapy by Kim Ernstmeyer.png" by Kim Ernstmeyer for Chippewa Valley Technical College is licensed under CC BY 4.0 ↵
- Nelson, K. J. (2021). Pharmacotherapy for personality disorders. UpToDate. https://www.uptodate.com ↵
- Nelson, K. J. (2021). Pharmacotherapy for personality disorders. UpToDate. https://www.uptodate.com ↵
- Nelson, K. J. (2021). Pharmacotherapy for personality disorders. UpToDate. https://www.uptodate.com ↵

