Community Health Nursing
Nurses working in a community setting include public health nurses, school nurses, and parish nurses, to name a few.
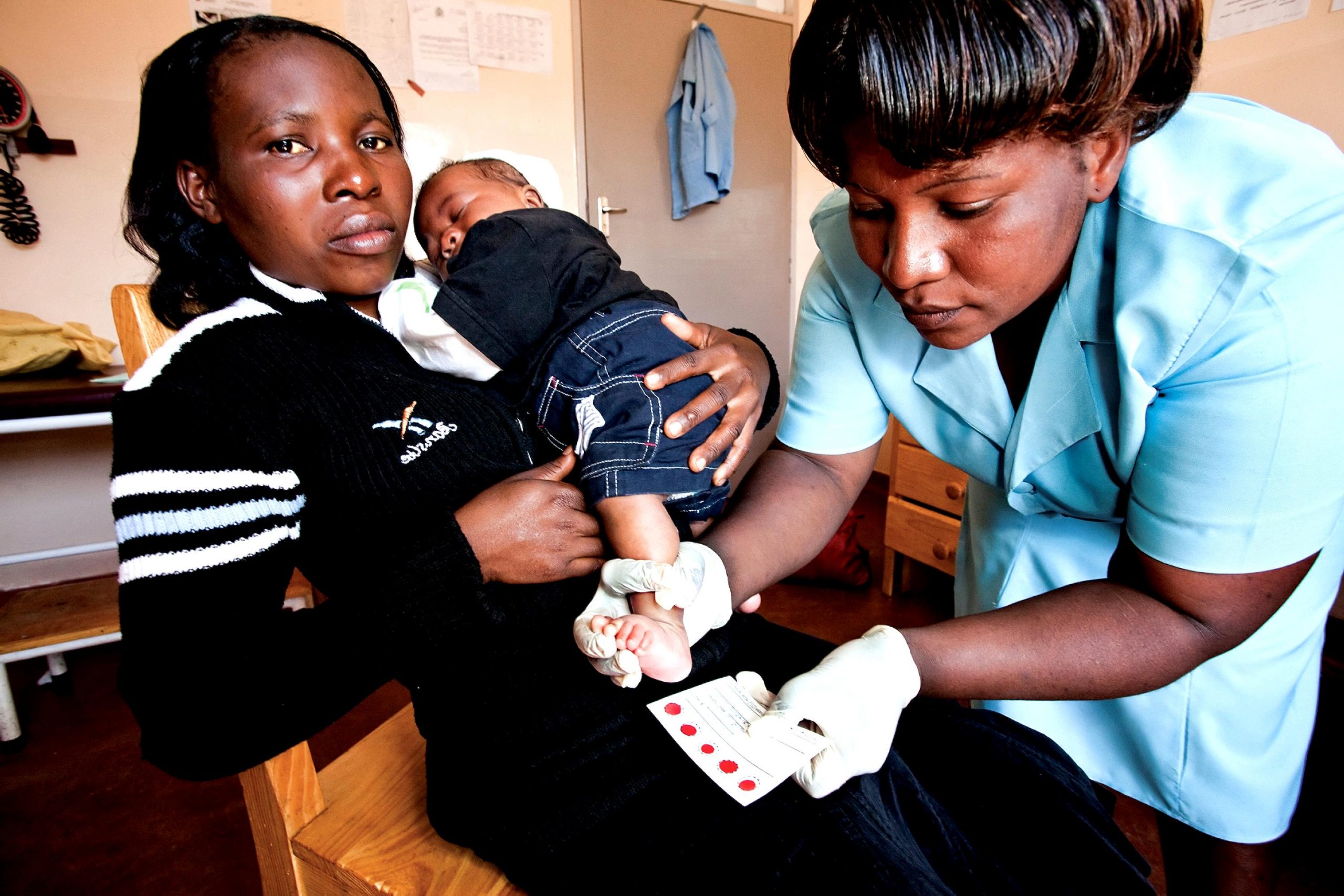
Public health nurses work across various settings in the community such as government agencies, community-based centers, shelters, and vaccine distribution sites. They provide disease prevention and health promotion services, such as working with mothers and children to improve nutrition, operating immunization clinics, and leading public health education initiatives such as smoking cessation campaigns. Public health nurses also prepare to respond quickly to public health emergencies such as natural disasters or epidemics.[1],[2] Emergency preparedness is further discussed in the “Environmental Health and Emergency Preparedness” chapter. See Figure 16.2[3] for an image of a community health nurse providing health screenings in a maternal and child health clinic.
School nurses work with over 56 million school-age children and adolescents. They provide direct care for chronic health problems and administer medications prescribed during school hours. They also provide mental health care, a need that has grown during the COVID-pandemic. Their work also affects the larger community. For example, school nurses may help develop disaster plans that coordinate activities in the school with the larger neighborhood.[4],[5]
Parish nurses use their nursing skills for church or parish members in paid or volunteer positions. They provide health education, screening, advocacy, and referrals to other services in the community.[6]
Barriers for Community Health Nurses
Community health nurses serve important roles in identifying priority health needs of a community, as well as planning and implementing preventative health initiatives. However, community health nurses may face unique barriers when providing care to individuals, families, and community members. Three barriers are referred to as gaining entry, role negotiation, and confidentiality:
- Gaining Entry: Community health nurses may be considered “outsiders” as representatives of the established health care system and may not necessarily be trusted by community members. It is vital for community health nurses to build trust and supportive relationships. When working with individuals and families, nurses should assess specific community issues affecting that individual’s health or their access to health care and then address those issues in their nursing care plan. Nurses can also investigate if there are community resources available to refer the client and/or their family members for additional services. See Figure 16.3[7] for an image of Red Cross volunteers working with caregivers of clients receiving palliative care.
- Role Negotiation and Confidentiality: Community health nurses must separate their roles as data collectors, health professionals, and neighbors. These roles can be difficult to differentiate when the nurse is assessing community health needs and providing nursing interventions for a population of individuals within their own home community. These individuals may include family members, friends, neighbors, or peers. Trust must be established and confidentiality assured according to legal and ethical parameters of nursing practice. Nurses should also establish a sense of partnership and encourage clients to participate in planning preventative health strategies for themselves and their families.

Community Health
Community health nursing is based on several underlying concepts such as encouraging healthy living, preventing illness, promoting rehabilitation, evaluating the effectiveness of community resources, and advocating for improved overall community health.[8],[9] In this manner, community health nurses pursue health equity. Health equity means that everyone has a fair and just opportunity to be as healthy as possible. This requires removing potential obstacles to obtaining and maintaining optimal health such as lack of access to health care services, good jobs with fair pay, quality education and housing, and safe environments.[10] Community health nurses address these conditions that are also known as social determinants of health.
Social determinants of health (SDOH) are the conditions in which people are born, grow, work, live, and age. Research shows that the SDOH can be more important than health care or lifestyle choices in influencing health and account for 30-55% of health outcomes.[11] See an illustration of SDOH in Figure 16.4.[12] SDOH can contribute to health inequities, defined as avoidable differences in health status seen within and between communities. In countries at all levels of income, health and illness follow a social gradient: the lower the socioeconomic position, the worse the health. According to the World Health Organization, SDOH can influence health equity in positive and negative ways[13]:
- Income and social protection
- Education
- Unemployment and job insecurity
- Working life conditions
- Food insecurity
- Housing, basic amenities, and the environment
- Early childhood development
- Social inclusion and nondiscrimination
- Structural conflict
- Access to affordable health services of decent quality

Health disparities are health differences that are linked with social, economic, and/or environmental disadvantages. Health disparities adversely affect groups of people who often experience greater obstacles to health based on individual characteristics such as socioeconomic status, age, gender, culture, religion, mental illness, disability, sexual orientation, or gender identity.[14] These groups are often referred to as “vulnerable groups,” and their care is further discussed in the “Vulnerable Populations” chapter.
As community health nurses strive to promote health equity, they assess SDOH, health disparities, and health inequities that are present in communities. They often begin by analyzing the context of the community because these characteristics can affect how community members respond to public health initiatives. The context of a community includes the following factors:
- Physical aspects: What geographical and man-made structures exist within the community? How do they shape the community’s access to health care and other institutions within the community? How do they shape the community health nurse’s access to the community members?
- For example, is this a rural community that requires long-distance transportation to health care services?
- Infrastructure: In what condition are the local roads, bridges, and highways? Is there public transportation available for community members to use to access health care services, grocery stores, schools, and other institutions providing basic needs? Do members of the community have access to the Internet, electricity, landline phones, cellular phone towers, and other technology?
- For example, are there buses or ride share services available for members to reach health care services?
- Patterns of settlement, commerce, and industry: How are residential and commercial areas located in the community? Are some residential areas located next to heavy industry? Are there areas of the community with higher crime rates? Are there areas defined by economic status within the community?
- For example, is there an area of the community located next to a factory contributing to air pollution?
- Demographics: What are the ages, gender, sexual orientation, race, ethnicity, marital status, education, and first language of the members of the community? What is the average number of people living in a household in the community?
- For example, is there an area where it is common for several multi-generation family members to live together in one residence?
- History: What local long- and short-term history affects the population of the community? What makes the community proud? What events in the community have helped shape the identity of the community members?
- For example, do public parks commemorate war veterans?
- Community leaders, both informal and formal: Who are the elected officials in the community, and what are their roles and relationships to the members of the community? Are there other informal leaders, such as church leaders, academic leaders, corporate CEOs, community activists, medical professionals, or others who serve an important role in the community? What are their roles and relationships to those in the community?
- For example, what relationships do the school board members have with community members?
- Community culture, both informal and formal: What are the spoken and unspoken rules and traditions of the community?
- For example, does the community have a tradition of celebrating Memorial Day with a parade and public tributes at a local cemetery?
- Existing groups and organizations: What adult, youth, and community groups and organizations exist that can be used to help build alliances and collaboration within the community?
- For example, is there a YMCA or other services in the community that promote physical activities for youth and other members of the community?
- Existing institutions: Where are the hospitals, medical care facilities, educational institutions, libraries, and religious institutions that serve the community? Are they accessible by public transportation? Who are the leaders in these institutions?
- For example, is there an urgent care clinic in this community that can be accessed by bus service?
- Economics: Where do most of the community members work? Do any businesses or industries form a base industry in the community? How is wealth distributed? What is the community’s average economic status: wealthy, upper middle class, working class, or poor?
- For example, is this a working class community whose members primarily work in a few local factories?
- Government/Politics: Are political leaders highly influential in the community? How do they serve their role in relationship to the members of the community? Does political power lie with others in the community?
- For example, how does the mayor of this city communicate with members of the community?
- Social structure: How do community members relate to one another on a routine basis? How are problems solved (or not solved) within the community? What symbols of respect and social relationships are evident?
- For example, is there a town board that meets regularly and collaboratively makes decisions affecting planning and zoning of the community?
- Attitudes and values: What does the community care about? What issues does it ignore? What assumptions can be observed about how community members believe people should relate to one another, dress, communicate, do business, or treat one another? Is there evidence of discrimination of a particular group of individuals within the community? What norms exist for interacting with members of the community who look or behave “differently” than others?
- For example, is it assumed in this community that neighbors will help clean up the neighborhood after storm damage occurs to several homes?
According to the CDC, a healthy community is one in which local groups from all parts of the community work together to prevent disease and make healthy living options accessible. Working at the community level to promote healthy living brings the greatest health benefits to the greatest number of people. It also helps to reduce health gaps caused by differences in income, education, race and ethnicity, location, and other factors that can affect health.[15]
Community Health Needs Assessment
Community health needs assessment is a systematic process to identify and analyze community health needs and assets in order to prioritize these needs, plan, and act upon significant unmet community health needs.[16] A community health assessment gives nurses and community organizations comprehensive information about the community’s current health status, needs, and issues. This information can be used to develop a community health improvement plan by justifying how and where resources should be allocated to best meet community needs.[17] Community health needs assessments are performed and reported at national, state, county, and local levels.
National Health Needs Assessments
Healthy People 2030 addresses the most current national public health priorities. It is published by the United States Department of Health and Human Services Office of Disease Prevention and Promotion. See Figure 16.5[18] for an illustration related to using Healthy People 2030 objectives and leading health indicators to assess community needs data, plan, and evaluate community health interventions.

A set of evidence-based Healthy People objectives are published every ten years based on current national data. Objectives are classified by categories[19]:
- Health Conditions
- Health Behaviors
- Populations
- Settings and Systems
- Social Determinants of Health
Examples of Healthy People 2030 community objectives include the following[20]:
- Increase the number of community organizations that provide preventative services
- Increase the rate of bystander CPR and AED use for nontraumatic cardiac arrests in public places
- Increase the proportion of adult stroke survivors who participate in rehabilitation services
Leading Health Indicators (LHIs) are a subset of high-priority Healthy People 2030 objectives to drive action toward improving health and well-being. Most LHIs address important factors that impact major causes of death and disease in the United States. They help organizations, communities, and community health nurses focus their resources and efforts to improve the health and well-being of all people. There are 23 LHIs that cover the life span from infants, children, adolescents, adults, and older adults. See a list of LHIs in Table 16.2.
Table 16.2 Leading Health Indicators Across the Life Span
| Life Stage | Leading Health Indicator |
|---|---|
| Infant |
|
| Children and Adolescents |
|
| Adults and Older Adults |
|
| All Ages |
|
Healthy People 2030 Resources
View Healthy People 2030 Objectives, Community Objectives, and Leading Health Indicators.
State Needs Assessments
States perform health needs assessments to develop state funding and program priorities for community health. For example, the Wisconsin Department of Health Services (DHS) performs a mental health and substance abuse needs assessment every other year. Data in this report includes the following:
- Prevalence of Needs: The prevalence of disorders, conditions, and associated problems for the entire population and subpopulations
- Access to Services: Determination of which and how many services are received by individuals and exploration of barriers to access
- Service Workforce and Capacity: Examination of the mental health and substance use services workforce, including the number of providers of these services and the geographic dispersion of the workforce across the state
Another example of a state needs assessment related to mental health is the Behavioral Health Gaps Study funded by the Wisconsin DHS to assess gaps and needs in the behavioral health service system for individuals with mental health and substance use disorders. Key gaps documented in this study included shortages in child and geriatric psychiatrists; shortages in mental health inpatient beds and residential facilities for treating substance use; inadequacies of the medical transportation system; a need for improving crisis stabilization services in the community that focus on reducing contact with police officers; shortages in medication-assisted treatment providers and clinics; long waitlists across the service array; shortages in competent translation services; and the need to provide wraparound services, particularly for consumers with families.[21]
Explore your state’s health needs assessments. Examples of health needs assessments in the state of Wisconsin are as follows:
Department of Health Service’s Mental Health and Substance Abuse Needs Assessment PDF
The Behavioral Health Gaps Report for the State of Wisconsin PDF completed by University of Wisconsin-Madison Population Health Institute
County Health Rankings
County health rankings are created annually by the University of Wisconsin Population Health Institute for counties across the country.[22] These rankings provide a snapshot of a community’s health and can be used as a starting point for implementing change to promote health equity in communities. See the following box to explore the health ranking for your community.
Visit the Explore Health Rankings web page from the University of Wisconsin Population Health Institute to view the health ranking of your community.
Local Needs Assessments
Local communities perform health needs assessments and develop specific health initiatives for their community members. For example, the Eau Claire County Health Department Needs Assessment was used to create a county health plan. In 2021 the top health priorities were documented as drug use, mental health, alcohol misuse, obesity, and healthy nutrition. See Figure 16.6[23] with an image related to data from a county mental health needs assessment.
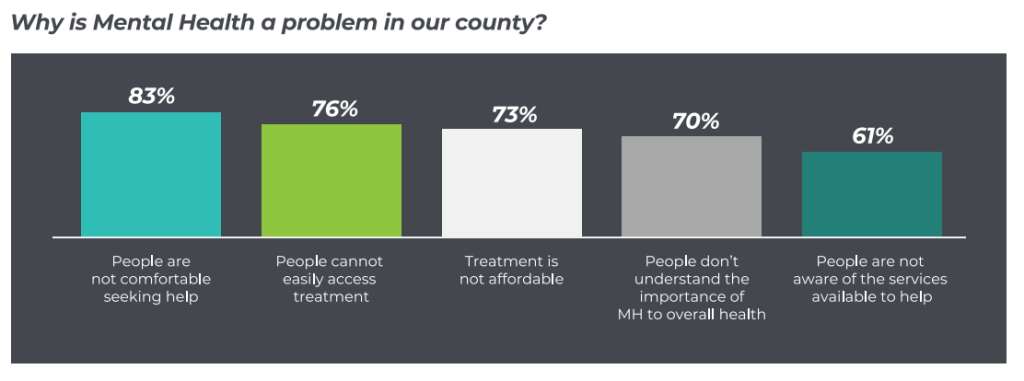
Explore your community’s health initiatives. View the example of Eau Claire City-County Health Department Needs Assessment.
Hospitals’ Community Health Needs Assessments
Tax-exempt hospitals are required to conduct community health needs assessments according to the Patient Protection and Affordable Care Act (i.e., the Affordable Care Act). Hospitals are required to adopt implementation strategies to meet the community health needs identified through their needs assessment. This collaboration among hospitals and community partners expands the community’s capacity to address health needs through a shared vision and creates a foundation for coordinated efforts to improve community health.[24]
View examples of hospitals’ community health needs assessments:
Mayo Clinic’s Community Health Needs Assessment PDF
Community Health Needs Assessments by HSHS Affiliated Hospitals in Wisconsin and Illinois
- Greenwood, B. (2018, June 29). What are the primary roles of the community nurse? CHRON. https://work.chron.com/primary-roles-community-nurse-15144.html ↵
- National Academy of Medicine. (2021, May). The future of nursing 2020-2030: Charting a path to achieve health equity [Report]. https://www.phnurse.org/assets/docs/FON%20Valuing%20Community%20and%20Public%20Health%20Nursing.pdf ↵
- “PIXNIO-45563-3000x2000” by USAID on Pixnio is licensed under CC0 ↵
- Greenwood, B. (2018, June 29). What are the primary roles of the community nurse? CHRON. https://work.chron.com/primary-roles-community-nurse-15144.html ↵
- National Academy of Medicine. (2021, May). The future of nursing 2020-2030: Charting a path to achieve health equity [Report]. https://www.phnurse.org/assets/docs/FON%20Valuing%20Community%20and%20Public%20Health%20Nursing.pdf ↵
- Greenwood, B. (2018, June 29). What are the primary roles of the community nurse? CHRON. https://work.chron.com/primary-roles-community-nurse-15144.html ↵
- “10716898813_74292ef548_k” by Department of Foreign Affairs and Trade is licensed under CC BY 2.0 ↵
- Greenwood, B. (2018, June 29). What are the primary roles of the community nurse? CHRON. https://work.chron.com/primary-roles-community-nurse-15144.html ↵
- National Academy of Medicine. (2021, May). The future of nursing 2020-2030: Charting a path to achieve health equity [Report]. https://www.phnurse.org/assets/docs/FON%20Valuing%20Community%20and%20Public%20Health%20Nursing.pdf ↵
- Braveman, P., Arkin, E., Orleans, T., Proctor, D., & Plough, A. (2017, May 1). What is health equity? Robert Wood Johnson Foundation. https://www.rwjf.org/en/library/research/2017/05/what-is-health-equity-.html ↵
- World Health Organization. (n.d.). Social determinants of health. https://www.who.int/health-topics/social-determinants-of-health#tab=tab_1 ↵
- “Healthy People 2030 SDOH Graphic.png” by U.S. Department of Health and Human Services, Office of Disease Prevention and Health Promotion is in the Public Domain. Access for free at https://health.gov/healthypeople/objectives-and-data/social-determinants-health ↵
- World Health Organization. (n.d.). Social determinants of health. https://www.who.int/health-topics/social-determinants-of-health#tab=tab_1 ↵
- HealthyPeople.gov. (2022, February 6). Disparities. Office of Disease Prevention and Health Promotion, U.S. Department of Health and Human Services. https://www.healthypeople.gov/2020/about/foundation-health-measures/Disparities ↵
- Centers for Disease Control and Prevention. (2015, September 18). A healthy community is a prepared community. [Blog]. https://blogs.cdc.gov/publichealthmatters/2015/09/a-healthy-community-is-a-prepared-community/ ↵
- Vigna, A. J. (2020). The 2019 behavioral health gaps report for the state of Wisconsin. University of Wisconsin Population Health Institute. https://uwphi.pophealth.wisc.edu/publications-2/evaluation-reports-2/. ↵
- VHA Inc., & Healthy Communities Institute. (2013). Assessing & addressing community health needs. Catholic Heart Association of the United States. https://www.chausa.org/docs/default-source/general-files/cb_assessingaddressing-pdf.pdf?sfvrsn=4 ↵
- “HP2030_HowtoUse_Screen1_2020-03-24.png” by unknown author for U.S. Department of Health and Human Services is in the Public Domain. Access for free at https://health.gov/our-work/national-health-initiatives/healthy-people/healthy-people-2030/promoting-healthy-people-2030. ↵
- Office of Disease Prevention and Health Promotion. Healthy People 2030: Building a healthier future for all. U.S. Department of Health and Human Services. https://health.gov/healthypeople ↵
- Office of Disease Prevention and Health Promotion. Healthy People 2030: Building a healthier future for all. U.S. Department of Health and Human Services. https://health.gov/healthypeople ↵
- Vigna, A. J. (2020). The 2019 behavioral health gaps report for the state of Wisconsin. University of Wisconsin Population Health Institute. https://uwphi.pophealth.wisc.edu/publications-2/evaluation-reports-2/. ↵
- Vigna, A. J. (2020). The 2019 behavioral health gaps report for the state of Wisconsin. University of Wisconsin Population Health Institute. https://uwphi.pophealth.wisc.edu/publications-2/evaluation-reports-2/. ↵
- This image is derived from 2021 Eau Claire County Community Health Assessment by Community Health Assessment Planning Partnership Committee and is in the Public Domain ↵
- VHA Inc., & Healthy Communities Institute. (2013). Assessing & addressing community health needs. Catholic Heart Association of the United States. https://www.chausa.org/docs/default-source/general-files/cb_assessingaddressing-pdf.pdf?sfvrsn=4 ↵
Nurses who work across various settings in the community such as government agencies, community-based centers, shelters, and vaccine distribution sites.
Nurses who provide direct care for children with chronic health problems and administer medications prescribed during school hours.
Nurses who use their skills for church or parish members in paid or volunteer positions.
Everyone has a fair and just opportunity to be as healthy as possible.
Conditions in which people are born, grow, work, live, and age.
Avoidable differences in health status seen within and between communities.
Health differences that are linked with social, economic, and/or environmental disadvantages.
Local groups from all parts of the community work together to prevent disease and make healthy living options accessible.
Systematic process to identify and analyze community health needs and assets in order to prioritize these needs, plan, and act upon significant unmet community health needs.

