4. “Treat the patient, not the monitor” — The Hospital Stay
What you are going to read now is a chapter that has a regular beginning, an awful middle, and, thankfully, a happy ending. In hindsight, some parts also offered a “foretaste of the feast to come,” but most of it felt like being on a reality TV show without even trying!
On Monday, August 10, 2020, the day before my 53rd birthday, the same friend and colleague who had accompanied me on the day of the biopsy took me to the hospital in the morning. We arrived a few minutes early, checked in, and went up to the surgery ward. I put on an ugly hospital gown and even uglier housecoat, had my vitals checked, and got a Covid-19 test done. Then we chatted about work-related matters for the most part, waiting patiently for my anesthesiologist and oncologist to meet us.
Upon hearing that I could not have a family member with me, the nurses decided to let my friend stay with me until about five minutes before they rolled me into the operating room. My anesthesiologist then administered an epidural, which hurt more than I had expected. I remember thinking, “I feel sorry for all those women in labour!”
I closed my eyes, asked the universe to look after me during the operation, and went to sleep.
When I opened my eyes six hours later, the nurses asked me for my full name and, according to my twin sister, whom they called after I had been taken to the recovery room, I was joking with them. While that sounds just like me, I have no recollection of it at all. In fact, all I remember is that for the next seven hours, I had my eyes closed (for the most part), but was, in fact, fully awake and listening to every word that was said; this is also what happens when I am on plane rides, regardless of the length.
As a result, I got more and more worried: my blood pressure was apparently tanking, especially the lower number, which refused to rise above 40. The nurses soon called my anesthesiologist, who said I had lost a lot of blood during the surgery (“What?!” I thought). Then she rattled off a list of drugs to give me and left for the day.
When my condition failed to improve within the hour, the nurses contacted the anesthesiologist on call for a second opinion. She checked me out, got really upset with her colleague for bombarding my body with (unnecessary?) medicine, and shouted “Let’s treat the patient, not the monitor” before she stomped out of the recovery room.
I did not know what to make of what had just happened, and neither did my nurse, who then decided to call another doctor for a third opinion. This white-haired gentleman patted me on the shoulder and then announced that both of his colleagues were wrong.
“She’s not sick enough to go to ICU,” he declared. “But she is not well enough to go to the ward either.”
Consequently, I was going to be sent to the medical surveillance unit for observation first.
At that time, I opened my eyes and said to the nurse, “Please call my twin sister and tell her about this change of plan.” She hesitated at first, but when I noted that it was close to midnight and this was a birthday wish, she readily agreed. I was stunned and angry, however, when she described my current state to my sister as “just fine” (?!), but there was nothing I could do about it either, so I let it go.
Another nurse and an aide then started pushing me out of the recovery room. I asked them for the time.
“It’s 11:55 pm — why do you want to know?”
“Because I am going to be 53 years old at midnight.”
They promptly launched into an off-key version of a tune I knew all too well.
Happy birthday to me
Hooked up to a multitude of machines, I decided there was absolutely nothing to celebrate at the hospital. My left arm was being squeezed every 15 minutes by a blood pressure cuff, a patient across the hall kept screaming “Help me, help me!”, and a nurse came in twice to take blood from my feet because there were no veins left in either of my arms (!). I was also getting increasingly annoyed with being asked to rate my pain by the night nurse.
“Still 10 out of 10,” I said. “Which part of that do you not understand?” I snapped at her. Had they run out of painkillers in this place of healing, or what was going on…?
When sunlight flooded my room in the morning, I realized that someone had written a congratulatory note on a board on the wall across from my bed. “It’s going to be one hell of a birthday,” I thought, wincing when a new nurse came in and lifted the flat sheet on top of me to check out my belly.
Heavy fatigue set in, which felt like 500 tractors slowly rolling up and down my body. When the oncologist resident came by to see me early in the morning — with Starbucks cake pops in hand as a present — I put up a brave front. In reality, I was ready to lose my mind. Were there no physicians in this hospital who were authorized to give me something for the pain?
“Hello, my dear,” a doctor with a booming and annoyingly cheerful voice said. “How are you feeling?”
“Awful,” I said, cussing under my breath in German first. Then I waited for him to offer a medical rationale as to what was going on. He did: part of my epidural had not worked.
“It happens,” he said matter-of-factly.
Upon finding out that I was a music history professor, the doctor dashed away, only to return with an iPad in hand. Soon a “Best of Baroque” recording was playing on YouTube. “Maybe he knows what he is doing after all,” I had to admit, smiling for the first time on my birthday.
But there was a price to pay — he wanted me to have some breakfast. Specifically, he wanted me to drink a half a bottle of Ensure. “I’ll try,” I said.
Then, I promptly threw up all over him.
“Oh @#$%,” I thought, feeling too weak to apologize.
“Oh dear,” he commented, asking the nurse to increase my nausea medication before he left.
I decided to pass the time by responding, albeit briefly, to the many “Happy Birthday” wishes I had received on my phone as texts and as messages on social media. One wish was even delivered in person that afternoon by one of my pastors, together with a beautiful prayer of hope.
It worked, as the night was (mostly) bearable. The colleague-friend who had dropped me off at the hospital visited the next morning; what a gift during Covid-19 times! I promised to try a bit of the opera cake (“How appropriate!” I thought) she had brought with her once I had been moved up to the “Short Stay” Ward. Two new “friends” were going to come along — a catheter and a plastic bulb which captured other bodily fluids, both of which needed draining on a regular basis. “I am never going to get any sleep,” I remember thinking.
You will be going home soon
My new room had the most depressing lack of natural light and came with a roommate I could not see as curtains were drawn all around my bed. Then, an unexpected gift arrived: a former colleague and fellow cancer survivor, who had moved to Montreal several years ago, had sent a huge box of delectable chocolates! They lifted my otherwise foul mood immediately, and it felt good to gift them to the nurses to show my appreciation for their hard work.
At lunch time, the emergency doctor with the booming voice wanted to watch me eat solid food — a decision he regretted shortly after when I threw up all over him again.
My oncologist and her resident also dropped by later that afternoon to inform me that they had found only one cancer (endometrial, i.e., uterine) which had spread to the ovaries; all lymph nodes had also been removed as a precaution. I would receive a call in about two weeks to tell me about the stage of the cancer. “That’s good to know,” I said.
Then, the oncologist confidently announced that I was going to go home the next day.
“Is she crazy?” I thought.
Surely, the nurses had told her that they had tried to get me to stand up four times, only for me to get super-dizzy and practically faint on the bed every single time. “We are all praying for you,” my sisters in B.C. and Germany as well as my pastor friend in Alberta said on the phone. They were all worried that I was not improving more quickly.
I finally started feeling better in the evening when my hidden roommate asked whether I wanted to listen to some hymns that had been recorded by musicians at her church. To our mutual delight, it turned out that I knew the pianist, a current student. She was also acquainted with a retired colleague of mine who contacted me that evening and offered to accompany me to my first chemotherapy treatment. Small world!
Having been awakened several times during the night to have my two “friends,” the bulb and the catheter, administered to, I was back to feeling awful the next morning.
“Now 699 tractors are running over my body!” I told my twin sister on the phone.
“Be patient,” my oncologist was quick to say when she visited.
She also reminded me that I had just undergone major surgery, lost a lot of blood, and needed to give my body time to heal. That was, incidentally, exactly what my oldest sister had told me the night before.
“Fair enough,” I thought, only to be stunned when the oncologist proceeded to tell me that I was going to be discharged soon.
“She is crazy,” I concluded.
“Why don’t you take a page out of the anesthesiologist’s book and treat me, the patient, not the monitor?” I snapped at her and her resident (and apologized for it the next day).
Whining to my family and friends at different times and across various time zones did little to lift my spirits either. Being moved over to the window spot after my roommate was discharged after lunch finally brought some relief.
How I had missed seeing the sun and blue skies!
Getting up to get out
“Change your attitude, or you will stay here forever” was the message my main guide — the one with the top hat — sent me seemingly out of the blue later that afternoon. I promptly pressed the red button to get the staff’s attention.
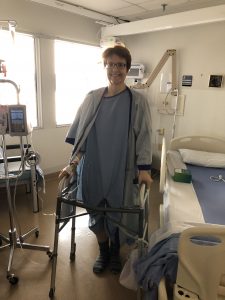
“I’d like to get up,” I said.
“I’ll help you,” the nurse replied. Gritting my teeth and using sheer will power, I did!
“Excellent; you keep that up,” she encouraged me.
“I will!”
I knew I had turned another corner when I put on music by my favourite composer a little later and began to relax despite of the uncomfortable hospital bed. Then, I asked whether it was possible to wash my hair. It involved a wet shower cap with shampoo on the inside and felt heavenly.
The next day, I amazed everyone — including two nursing students who had done a great job earlier cleaning my huge scar — first, by getting out of bed to sit in the chair next to the window, and then, by using a walker to circle the ward twice. A physiotherapist who introduced himself in the hallway, followed me to my room. “You were clearly in excellent shape before you had surgery,” he said.
“I plan to bounce back in record time,” I replied.
It still took several days to be well enough to leave the hospital. On the weekend, I kept pestering the nurses about being discharged, but not before they had removed my catheter and bulb “friends,” as I was not willing to take them home with me. In turn, the nurses kept bugging me to eat more and get my digestion going.
“I would love to — if only I could prepare the food myself,” I said. To prove my point, I sent my twin sister a picture of what had been sent up for lunch; I had ordered it from a list provided by a dietician the day before. My sister was unable to identify any of the dishes, much to my delight.
“According to the printout, the yellowish bit is supposed to be chicken pot pie, and the green liquid is listed as turkey soup,” I informed her. Thankfully, another colleague-friend — a fellow German who, incidentally, one of the nursing students recognized as her biology professor — visited on Saturday and Sunday. She brought two bags of sweet treats with her, one of which I shared with the staff, much to their delight.
Finally, on the morning of Tuesday, August 18, 2020, over a week after I had undergone surgery, I was told that I would be discharged after lunch. Hallelujah! Waiting for my oncologist to make it official, I circled the ward again and again, quietly sending love and gratitude to everyone who had been praying for my speedy recovery.
Then, a nurse told me what to expect over the course of the next month or so. My oncologist would call me about the stage of my cancer in two weeks and do a follow-up exam three weeks later; my first of six chemotherapy appointments had been booked for September 25, 2020. Until then, I was to take it easy and try to gain some of the weight back that I had lost because of the surgery. “I’ll do my very best,” I promised.
Handing thank-you cards to my oncologist, her resident, and the staff, I grabbed my bag as well as the medication and blood thinner I was to take home with me and walked (!) down to the main entrance, where my colleague-friend was waiting.
“I expected you to be in a wheelchair,” she said.
“Not needed,” I replied.
However, the pillow on my belly during the ride home was a visual reminder that I had a lengthy recovery period ahead of me.

