13 Emergency Preparedness and Response
Yvonne Harris
We see all comers, from the worried well to the critically ill; from birth to death; and with conditions involving all parts of the mind, body, and spirit; from brain trauma to ingrown toenails. Our patients come to us trusting that we will respect their concerns and that we will provide care for them. As emergency nurses, we have a responsibility to respect that trust and provide our patients with the skill and expert knowledge required for their care.
—Jean Proehl (2009, p. xi)
Introduction
Emergency nurses see it all. Disasters have claimed millions of lives and cost billions of dollars worldwide in the past few decades. Goodwin Veenema suggests that there is, on average, a disaster requiring international assistance every week (2013). Tragedies such as the September 11th World Trade Center attacks, Hurricane Katrina, and the 2010 earthquake in Haiti have led heath care providers to critically review their processes in order to deal with such events.
Figure 13.1 Waiting to be Rescued after Hurricane Katrina, New Orleans

Nurses need to be familiar with their role in emergency preparedness and disaster planning as they frequently have wide-ranging leadership responsibilities for community- and hospital-level disaster preparedness and response. This chapter discusses the definition of a disaster, either natural or anthropogenic (caused by humans), disaster preparedness and planning, and the disaster response.
Learning Objectives
- Discuss the four areas of focus in emergency and disaster planning—mitigation, preparedness, response, and recovery.
- Describe the core preparedness actions.
- Recognize situations that may call for additional comprehensive planning.
13.1 Disaster
Disasters are defined in many ways. The World Health Organization (WHO, n.d.) defines disaster as “a situation or event, which overwhelms local capacity, necessitating a request to the national or international level for external assistance.” The United States Department of Homeland Security (USDHS) defines it as an emergency that “requires responsive action to protect life or property” (USDHS, 2008, p. 138). Hammond, Arbon, Gebbie, & Hutton (2012) summarize these definitions in their statement that
A disaster is a serious disruption of the functioning of a community or a society involving widespread human, material, economic or environmental losses and impacts, which exceeds the ability of the affected community or society to cope using its own resources.” (p. 236)
Simply put, a disaster is a catastrophic event that overwhelms available resources. Disasters can be natural or anthropogenic (caused by human activity). In May 2016, a fire in Fort McMurray, Alberta, destroyed 2,400 structures in the area, forcing more than 90,000 people to evacuate the region.
The fire grew so much that at one point it was creating its own weather and required firefighting reinforcements from across the country. All the stores and amenities in Fort McMurray were closed . . . and residents were told to boil their water. (Morgan, 2016)
Figure 13.1.1 Highway 63 near Fort McMurray, Alberta, May 3, 2016

Natural disasters such as tornadoes, earthquakes, floods, and extreme winter conditions occur more frequently than anthropogenic disasters such as civil unrest, terrorism, and armed conflict; in 2015, there were 376 naturally triggered disasters registered (Guha-Sapir, Hoyois, & Below, 2015). Disasters are typically considered “low probability, high impact” events (Saunderson Cohen, 2013, p. 21).
Planning for any type of disaster requires consideration of common elements including mitigation, preparedness, response, and recovery. Canada’s Emergency Management Act recognizes the roles that all stakeholders must play in Canada’s emergency management system including “coordinating emergency management activities among government institutions and in cooperation with the provinces and other entities” (Emergency Management Act, 2007).
13.2 Disaster Mitigation
Disaster mitigation measures are those that eliminate or reduce the impacts and risks of hazards through proactive measures taken before an emergency or disaster occurs. It begins with identifying the risks. Health care leaders need to evaluate potential emergencies or disasters that could impact the demand for their services and supplies, then develop a plan that will address those needs. Public Safety Canada describes the Red River Floodway as an example of disaster mitigation.
The building of the Floodway was a joint provincial/federal undertaking to protect the City of Winnipeg and reduce the impact of flooding in the Red River Basin. It cost $60 million to build in the 1960s. Since then, the floodway has been used over 20 times. Its use during the 1997 Red River Flood alone saved an estimated $6 billion. The Floodway was expanded in 2006 as a joint provincial/federal initiative. (2015)
Hendrickson & Horowitz, (2016) explain that hospital facility planners and health leaders should address those disasters that are most likely to occur in their community and geographic area and perform a hazard vulnerability analysis to determine the likely vulnerabilities that may arise in their facility from those disasters.
A hazard vulnerability analysis (HVA) is defined as a systematic approach that:
- identifies all hazards that may affect a community;
- determines the probability of the hazard;
- determines the consequences of the hazard; and
- analyzes the findings to determine what hazards are of priority (Saunderson Cohen, 2013; Hendrickson & Horowitz, 2016).
For example, industrial sites that store large volumes of potentially harmful chemicals pose a hazardous material threat that could require mass decontamination. Area hospitals would need to have functional decontamination units, as well as an abundant supply of ventilators, oxygen, and specific antidotes that are not typically available in large quantities. Natural disasters often result in increased numbers of homeless or displaced persons whose everyday medical needs may be exacerbated by limited access to routine health care. This may result in emergency departments experiencing an influx of patients seeking medication, treatments, and assessments.
The results of an HVA can be used to develop and streamline disaster plans. These plans should be designed using an interdisciplinary approach, including partners from local police, emergency, and fire services. HVAs should be conducted on an annual basis, or whenever there are demographic or infrastructural changes that may impact the potential of a disaster.
13.3 Disaster Preparedness
Figure 13.3.1 Medical Crew Conduct Mass Casualty Scenario Drill
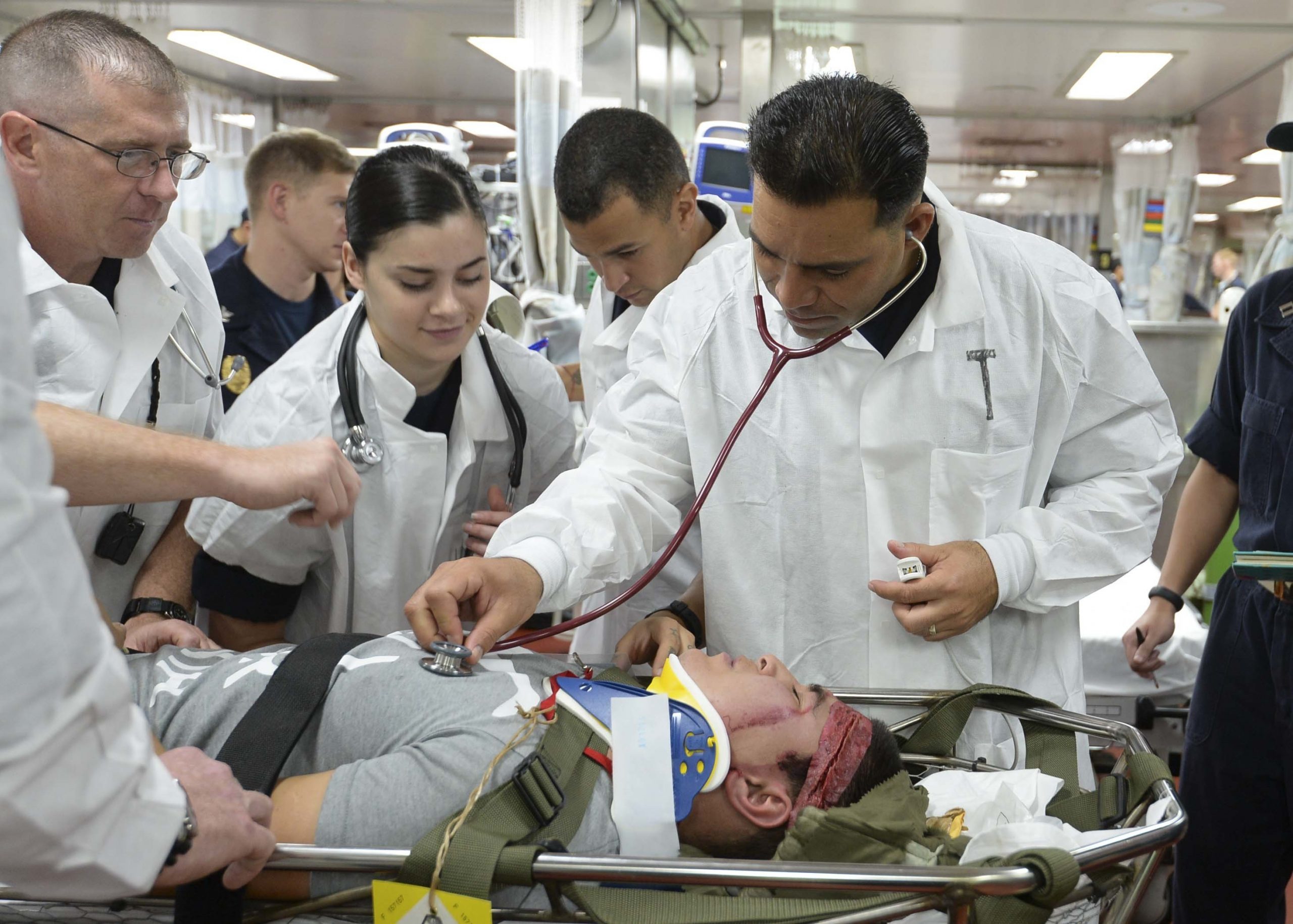
The goal of disaster preparedness is to plan a response that will decrease the damages and support the recovery from a disaster (Stopford, 2007). Nurses, with their expertise in primary health care, extensive experience with interdisciplinary teamwork, and strong collaborative skills are the ideal leaders in disaster preparedness. The first step in preparing for a disaster is developing a strategic emergency management plan (SEMP) (Public Safety Canada, 2016) in anticipation not only for those disasters that are most likely to occur in a specific geographical area, but also those that are unexpected (Saunderson Cohen, 2013).
The SEMP is a broad scope document that guides and informs partners internally and externally on how to respond to disasters. It includes specific processes for:
- the main goals of the plan and the method for attaining those goals;
- obtaining information on threats; and
- planning standard response to threats.
Essential Learning Activity 13.3.1
For detailed information on SEMP, refer to Annex A of the Emergency Management Planning Guide, 2010–2011, published by Public Safety Canada.
Stopford (2007) provides a comprehensive list of additional processes including:
1. Determining a command and control plan. When determining a line of command, it is essential to ensure you have both a command person and a second-in-command, should the situation arise that the primary commander is unable to fulfill the role. The control plan must also include the designation of a specific location for the command centre.
2. Identifying the functional roles and responsibilities of internal and external agencies. Internal and external department need to have a clear understanding of both their roles and responsibilities and other parties’ roles and responsibilities during a disaster. Contact information of emergency personnel, along with their roles should be readily available. Additionally, essential service staff should be defined, thus ensuring that there is consistent emergency staff coverage during the disaster.
3. Determining a communication system. A standard process of communication must be developed to address the possibility of system failure. The contingency process should include the use of land lines, cellphones, and radios as standard communication equipment.
4. Confirming a legal basis for response to include isolation strategies as needed for infection control. Disaster preparedness must include details for the processes of isolation, infection control, and allocation of medications such as vaccines, antibiotics, and antiviral agents should they become short in supply. Additionally, should there be a need for facility lockdown and controlled facility access, legal and ethical concerns need to be considered when developing this portion of the plan.
5. Developing an infectious disease plan. Standard process needs to address the potential for an infectious disease outbreak or pandemic. Different illnesses require different levels of isolation and personal protective equipment (PPE). Disaster preparedness addresses the possibility of high-level isolation equipment requirements and ensures adequate supplies and equipment are readily available. Emergency care providers should be familiar with clinical signs of different diseases, and a surveillance methodology plan should be in place to address possible advancement of the disease process.
6. Obtaining and maintaining emergency facilities, equipment, and supplies. Emergency preparedness requires a standard process for obtaining and maintaining emergency equipment and supplies. This includes a standard maintenance schedule, a tracking schedule of where equipment is located, and details where to obtain additional equipment and supplies.
7. Providing disaster preparedness training for emergencies. Training may involve
- educating personnel to understand their role in an emergency;
- donning and doffing PPE;
- decontamination procedures; and
- triage.
Training should occur on a regular basis and should be included in regional orientation for all personnel. Individual facilities require additional planning on the steps to take if a disaster disrupts their day-to-day facility operations. This planning is directed at facility leadership and personnel and provides a standard process for ensuring facilities can continue to provide regular essential services (Saunderson Cohen, 2013). Additional considerations suggested by Stopford (2007) include planning for a lockdown of the facility. Staff may be required to remain in the facility, and if so, they need to be trained to develop a contingency plan for family emergency planning.
13.4 Disaster Response
The first step in responding to an incident is recognizing the event is occurring and initiating the plans that were developed in the preparedness phase. External responses may include activities such as search-and-rescue operations, firefighting, and building shelters for displaced persons. Nurses need to have a good understanding of the disaster plan, as well as a concrete awareness of the events surrounding the incident, to provide the best care for their patients. As an example, during the 2016 Fort McMurray fire, surrounding hospitals were required to be prepared to care for high numbers of patients with burns and respiratory compromise. This included not only the citizens, but also firefighters and first responders.
Efficient internal facility responses to disasters include disaster triage and casualty distribution (Saunderson Cohen, 2013). Nursing during a disaster often focuses on providing care to an influx of patients to a care centre, and it requires an understanding that these patients may have varying degrees of illness and injury as well as emotional stress from the event. Disaster triage is the process of “doing the greatest good for the greatest number of casualties” and has been characterized as the “keystone to mass casualty management” (Saunderson Cohen, 2013, p. 26).
Treatment priorities may vary according to available supplies and resources, as well as the type of disaster (Stopford, 2007).
Various disaster triage systems have been designed for use in mass casualty incidents; therefore, it is important for facilities to determine in advance which system they will use. One method of disaster triage is the simple triage and rapid transport (START) tool. This system was developed in the 1980s in Orange County, California, and has been adopted throughout many countries (Saunderson Cohen, 2013, p. 27).
When the triage nurse is using the START tool, patients are rapidly assessed (less than one minute) and determined to be either red, yellow, green, or black.
| RED |
Immediate care required. These patients are in a priority treatment category with illnesses or injuries that could result in loss of life or limb. |
| YELLOW |
Urgent care required. This category of patient requires urgent treatment but can wait until the red-tagged patients have been stabilized. |
| GREEN |
Minimal care required. These patients require care but are deemed stable enough to wait several hours for treatment. |
| BLACK |
End-of-life care required. Black-tagged patients are deemed to be beyond the ability of the care team to provide lifesaving care. They are in a state of impending death or already lifeless. |
Essential Learning Activity 13.4.1
Mass casualty incidents involving high numbers of pediatric patients use the JumpSTART system. Read about the process of triaging pediatric patients using the JumpSTART Pediatric Triage Algorithm from the US Department of Health and Human Services.
13.5 Disaster Recovery
Figure 13.5.1 Gratitude to Nurses

Disaster recovery follows the response phase and is defined by the short-term and long-term actions required to return the community to a normal state. Short-term recovery includes returning vital life support systems to an operational state and repatriation of patients. Establishing a protocol for the safe transport of patients back to their designated facility as soon as possible helps to alleviate the psychological trauma of family separation. Additionally, it eases the burden on the alternate care facilities and staff called into action during the disaster (Assid, 2014).
Long-term recovery includes such actions as restoring damaged infrastructure and damaged property, and providing physical and psychological support for victims, families, and responders (Upton, 2013). Physical damage is an easily identifiable visual cue of disaster, but it is not always present (Saunderson Cohen, 2013). Pandemics, bio- and cyber-terrorism are examples of disasters that leave minimal or no visual footprint. However, the psychological impact may last for years, for both patients and the health care team. Individuals who experience a traumatic event are at risk of suffering long-term effects, which. may be physical, emotional, spiritual, or mental. Characteristics of these responses include:
- emotional reactions to events;
- loss of ability to function;
- feeling overwhelmed; and
- increased use of resources.
Essential Learning Activity 13.5.1
Canada has had a number of major disasters over the past few years.
- Nurses played significant leadership roles during the Fort McMurray fires (mentioned earlier in this chapter) and in the follow-up recovery. Go to the links below, then answer the questions that follow.
“‘We got the job done’: Nurse describes Fort McMurray hospital evacuation” by Rob Drinkwater (Canadian Press, May 5, 2016)
“A year after the fire, Fort McMurray residents report an uneven recovery” by Keith Gerein (Edmonton Sun, April 25, 2017)
(a) What were the major issues facing nurses who evacuated the hospitals in Fort McMurray?
(b) What are the major health issues facing Fort McMurray residents as they recovered from the fire?
2. Read the following articles on the Lac-Mégantic train derailment titled “The public health response during and after the Lac-Mégantic train derailment tragedy: a case study,” then answer the questions that follow.
Généreux, M., Petit, G., Maltais, D., Roy, M., Simard, R., Boivin, S., Shultz, J. M., & Pinsonneault, L. (2014). The public health response during and after the Lac-Mégantic train derailment tragedy: A case study. Disaster Health, 2 (3–4), 113–120. doi:10.1080/21665044.2014.11031
(a) Describe the seven lessons learned by public health professionals.
(b) Why do public health actions continue long after emergency response operations have concluded?
3. Read the following sources for information on the role that nurses played during the 2003 SARS pandemic in Toronto, and the role that nursing leadership played in preventing further spread of the illness, then answer the questions that follow.
“Lessons learned from SARS” by Melissa Di Costanzo (Registered Nurse Journal, May/June 2013)
“SARS, 10 years later: One family’s remarkable story” by Amy Dempsey (Toronto Star, March 2, 2013)
(a) What were some of the long-term effects that nurses reported following the traumatic event?
(b) What were the primary lessons learned?
Research Note
Goodwin Veenema, T., Andrews, D, Losinski, S., Newton, S. M., & Seal, S. (2016). Exploration and development of standardized nursing leadership competencies during disasters. Health Emergency and Disaster Nursing, 4, 26–38.
Nash, T. J. (2016). A guide to emergency preparedness and disaster nursing education resources. Health Emergency and Disaster Nursing, 4, 12–25.
Canadian Nurses Association. (2010). Evidence-informed decision-making and nursing practice. [Position statement] Retrieved from http://cna-aiic.ca/~/media/cna/page-content/pdf-en/ps113_evidence_informed_2010_e.pdf
Imagine you are just finishing your day shift in the emergency department when the EMS radio patches in that a tornado has touched down in a community 50 kilometres outside the city. Numerous homes and businesses have been completely destroyed. EMS, fire, and police are on scene and have begun transporting patients to your ED. Are you prepared? Do you have the knowledge to provide the best care for the victims?
Evidence-based practice has always been part of the nursing lexicon; over the last few decades it has taken a more prominent role in nursing education (CNA, 2010). A broad scope of knowledge is needed to be an effective emergency nurse, which requires keeping current on the latest research about nursing and health care. However, research has shown that many nurses do not have the basic understanding or knowledge to prepare for a disaster. A literature review done by Nash (2016) suggests that nurses do not feel comfortable responding to disaster situations due to scarcity of emergency preparedness resources (p. 12). The challenge lies in the lack of current literature related to emergency nursing and disaster preparedness. Additional literature reviews strengthen this argument and contend that evidence-based leadership research is minimally available (Goodwin Veenema, Andrews, Losinski, Newton, & Seal, 2016, p.36). Clinical research in emergency nursing underpins the development of practice guidelines, such as door-to-needle and door-to-balloon times for treatment of acute coronary syndromes and family presence during resuscitation. Research in emergency preparedness is no exception.
The inevitability of future disasters, both natural and anthropogenic, combined with the currently limited resources related to education and training, means that there needs to be a greater focus on disaster preparedness education in nursing curricula. There is an opportunity for nursing education to forge the way for continued research, thereby meeting this continuing challenge.
Summary
Disasters are unpredictable and can occur anywhere, at any time. Nursing during a disaster requires a coordinated effort among professionals throughout the health care, public, and private service sectors.
Today’s nurses are faced with the challenges of responding to natural, anthropogenic, and technological disasters. Strong leadership is required to address the unique set of challenges and necessary preparation for such events. “When a disaster strikes a community—whether a bus accident, a tornado, a hurricane, or terrorist attack—nurses will be on the front lines helping those who are in need” (Knebel, as cited in Goodwin Veenema, 2013, p. xxvi). As the frequency, magnitude, and variety of disasters, both anthropogenic and natural, continue to escalate, nursing leaders will need to respond with “awareness, preparedness, political prowess…and most of all, teamwork on all levels” (Ford, as cited by Goodwin Veenema, 2013, p. xxix).
After completing this chapter, you should now be able to:
- Discuss the four areas of focus in emergency and disaster planning—mitigation, preparedness, response, and recovery.
- Describe the core preparedness actions.
- Recognize situations that may call for additional comprehensive planning.
Exercises
1. Watch this video titled “START Simple Triage and Rapid Treatment” (18:19) on START triage basics, then read the following simulated scenario:
You are on a ride-along with EMS and are first on the scene to a multi-vehicle collision on Highway 1 involving five passenger vehicles and one semi carrying non-hazardous materials. There are ten victims in various stages of crisis.
Triage the following victims using the START adult triage categories: green, yellow, red, and black.
(a) Female, 77 years, scalp avulsion, no spontaneous breathing
(b) Male, 45 years, ambulatory, RR 20, bleeding noted from scalp, asking if he can help
(c) Male, 30 years, no spontaneous breathing, impaled pipe through chest
(d) Male, 55 years, gasping respirations RR 32, bleeding from both arms
(e) Female, 27 years, non-ambulatory, RR 18, obeys commands
(f) Male, 23 years, RR 28/minute, large laceration to head, decreased LOC, not obeying commands
(g) Female, 44 years, limping, complaining of left knee pain, painful left arm. Obvious deformity of left arm, cap refill < 2 seconds, RR 24/minute
(h) Male, 79 years, walking between vehicles, calling for his wife, no obvious injuries
(i) Female, 19 years, ambulatory, c/o feeling dizzy, RR 16, no obvious injuries
(j) Female, 18 years, ambulatory, crying, RR 22, bleeding from nose
2. Several city hospitals create a network of policies and agreements governing the redirection of patients should one emergency department become overwhelmed beyond ability to respond. Which phase of the emergency management plan does this action exemplify?
(a) mitigation
(b) preparedness
(c) response
(d) recovery
3. Choose the statement which best describes the mitigation phase of a disaster event.
(a) Establishing a protocol for the safe transport of patients back to their designated facility as soon as possible occurs during the mitigation phase.
(b) The mitigation phase of disaster encompasses assessing physical and structural damages.
(c) Mitigation begins with identifying the risks.
(d) The mitigation phase of a disaster is the final phase of a disaster experience.
SOLUTIONS
1. (a) Female, 77 years, scalp avulsion, no spontaneous breathing (black)
(b) Male, 45 years, ambulatory, RR 20, bleeding noted from scalp, asking if he can help (green)
(c) Male, 30 years, no spontaneous breathing, impaled pipe through chest (black)
(d) Male, 55 years, gasping respirations RR 32, bleeding from both arms (red)
(e) Female, 27 years, non-ambulatory, RR 18, obeys commands (yellow)
(f) Male, 23 years, RR 28/minute, large laceration to head, decreased LOC, not obeying commands (red)
(g) Female, 44 years, limping, complaining of left knee pain, painful left arm. Obvious deformity of left arm, cap refill < 2 seconds, RR 24/minute (yellow)
(h) Male, 79 years, walking between vehicles, calling for his wife, no obvious injuries (green)
(i) Female, 19 years, ambulatory, c/o feeling dizzy, RR 16, no obvious injuries (green)
(j) Female, 18 years, ambulatory, crying, RR 22, bleeding from nose (green)
2. (b) Preparedness. Rationale: Establishing inter-hospital agreements and coordination arrangements prior to a disaster, constitutes a preparedness phase action.
3. (c) Mitigation begins with identifying the risks. Rationale: Disaster mitigation measures are those that eliminate or reduce the impacts and risks of hazards through proactive measures taken before an emergency or disaster occurs. It begins with identifying the risks.
References
Assid, P. A. (2014). Disaster management. In D. Gurney (Ed.), Trauma nursing core course (7th ed.), pp. 311–324. Des Plaines, IL: Emergency Nurses.
Canadian Nurses Association. (2010). Evidence-informed decision-making and nursing practice. Retrieved from http://cna-aiic.ca/~/media/cna/page-content/pdf-en/ps113_evidence_informed_2010_e.pdf on 9-December-2016
Emergency Management Act, S.C. 2007, c. 15 Retrieved from http://laws-lois.justice.gc.ca/PDF/E-4.56.pdf. Généreux, M., Petit, G., Maltais, D., Roy, M., Simard, R., Boivin, S., Shultz, J. M., & Pinsonneault, L. (2014) The public health response during and after the Lac-Mégantic train derailment tragedy: A case study. Disaster Health, 2, (3–4), 113–120. doi:10.1080/21665044.2014.11031
Goodwin Veenema, T., Andrews Losinski, S., Newton, S. M., & Seal, S. (2017). Exploration and development of standardized nursing leadership competencies during disasters. Health Emergency and Disaster Nursing, 4(1), 26-38. https://doi.org/https://doi.org/10.24298/hedn.2015-0016
Goodwin Veenema, T. (2013). Disaster nursing and emergency preparedness for chemical, biological, and radiological terrorism and other hazards (3rd ed.). New York, NY: Springer.
Guha-Sapir, D., Hoyois, P., & Below, R. (2015). Annual disaster statistical review 2015: The numbers and trends. Brussels: Centre for Research on the Epidemiology of Disasters. Retrieved from http://reliefweb.int/sites/reliefweb.int/files/resources/ADSR_2015.pdf
Hammond, K. S., Arbon, P., Gebbie, K., & Hutton, A. (2012). Nursing in the emergency department (ED) during a disaster: A review of the current literature. Australasian Emergency Nursing Journal, 15, 235–244. doi:10.1016/j.aenj.2012.10.005
Hendrickson, R. G., & Horowitz, B. Z. (2016). Disaster preparedness. In J. E. Tintinalli, J. S. Stapczynski, O. J. Ma, D. M. Yealy, G. D. Meckler, & D. M. Cline (Eds.), Tintinalli’s emergency medicine: A comprehensive study guide (8th ed.). Retrieved from http://accessmedicine.mhmedical.com/content.aspx?bookid=348§ionid=40381465
Morgan, G. (2016, December 29). Rebuilding in the wake of “the beast”; Massive effort ahead in Fort Mac. National Post. Retrieved from http://search.proquest.com/docview/1854096885?accountid=39725
Nash, T. J. (2016). A guide to emergency preparedness and disaster nursing education resources. Health Emergency and Disaster Nursing, 4, 12–25.
Proehl, J. A. (2009). Emergency nursing procedures (4th ed.). St. Louis, MO: Saunders Elsevier.
Public Safety Canada. (2016). Emergency management planning. Retrieved from https://www.publicsafety.gc.ca/cnt/mrgnc-mngmnt/mrgnc-prprdnss/mrgnc-mngmnt-plnnng-eng.aspx
Public Safety Canada. (2015). About disaster mitigation. Retrieved from https://www.publicsafety.gc.ca/cnt/mrgnc-mngmnt/dsstr-prvntn-mtgtn/bt-dsstr-mtgtn-en.aspx
Saunderson Cohen, S. (2013). Mass casualty incidents. In B. B. Hammond & P. Gerber Zimmerman (Eds.), Sheehy’s manual of emergency care (7th ed.), pp. 19–35. St. Louis, MO: Elsevier Mosby.
Stopford, B. M. (2007). Disaster preparedness and response. In K. S. Hoyt & J. Selfridge-Thomas (Eds.), Emergency nursing core curriculum (6th ed.), pp. 955–969. St. Louis MO: Saunders Elsevier.
Upton, L. A. (2013). Disaster. In Emergency nursing pediatric course: Provider manual (4th ed.), pp. 365–382. Des Plaines, IL: Emergency Nurses Association.
US Department of Homeland Security. (2008). National incident management system. Retrieved from https://www.fema.gov/pdf/emergency/nims/NIMS_core.pdf
World Health Organization definitions: emergencies. (n.d.). Retrieved from http://www.who.int/hac/about/definitions/en/


Feedback/Errata